Unstable Angina
Cardiovascular disease affects more people worldwide than any other condition. The heart's inadequate blood flow and oxygen supply cause unstable angina, which can lead to a heart attack without proper treatment. Unstable angina pectoris is different from its stable counterpart.
A patient's ability to spot early symptoms improves with knowledge of angina pectoris's pathophysiology. With this you can develop better prevention strategies and seek timely medical help. This article explains what unstable angina is and its causes, symptoms, and treatment options.
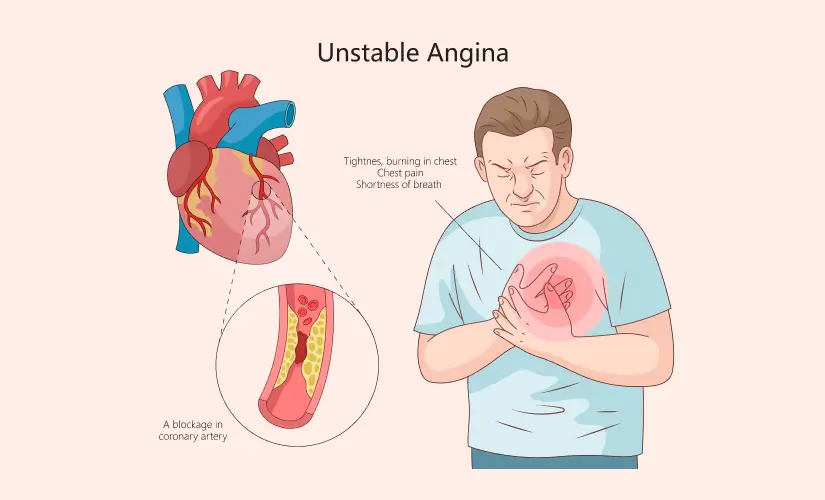
What is Unstable Angina?
The chest pain from unstable angina comes suddenly without following any pattern. This condition belongs to the spectrum of acute coronary syndromes. Critical narrowing of arteries that supply blood to the heart makes immediate emergency treatment necessary. It strikes without warning—during rest, sleep, or with minimal activity. The pain episodes usually last longer than 15 minutes and don't improve with rest or medication. This condition warns that a heart attack could happen soon.
Unstable Angina Symptoms
People with unstable angina might experience:
- Chest pain that feels tight, pressure-like, crushing, burning or sharp
- Pain that spreads to the jaw, arm, neck or back
- Shortness of breath
- Sweating
- Anxiety
- Dizziness
- Nausea and vomiting.
Causes of Unstable Angina
Coronary artery disease due to atherosclerosis causes most cases. Fatty plaque builds up along artery walls and restricts blood flow. Blood clots can also form on ruptured plaque and suddenly block arteries.
Risk Factors of Unstable Angina
Several factors raise your risk, including:
- Your risk increases after age 45 for men and 55 for women.
- History of a heart attack
- Diabetes
- Heart disease in your family
- High blood pressure
- Abnormal cholesterol levels
- Smoking
- Inactive lifestyle
- Obesity.
Diagnosis of Unstable Angina
Medical providers start with a full picture of your medical history and conduct a physical examination. They will listen to your heart for abnormal heart sounds and check for changes in blood pressure.
Diagnostic tests:
- Electrocardiogram (ECG) to detect heart electrical activity changes
- Blood tests checking for cardiac enzymes like troponin
- Chest X-ray to review heart condition
- Echocardiogram showing heart muscle function
In some cases doctors might order additional tests. These include:
- Stress tests to detect exercise-induced ischemia
- Cardiac catheterisation to directly assess blood flow
- Coronary angiography visualises the coronary arteries to detect blockages or plaque buildup.
Unstable Angina Treatments
Hospital emergency departments typically start the treatment process. Standard approaches are:
Medications:
- Aspirin and other antiplatelet drugs to prevent clotting
- Nitroglycerin to widen blood vessels
- Beta-blockers to decrease the heart workload
- Statins for cholesterol management
Doctors may recommend angioplasty with stent placement or coronary artery bypass surgery for severe cases.
Complications of Unstable Angina
Heart attack remains the biggest risk. Other complications include:
- Abnormal heart rhythms (arrhythmias)
- Heart failure
- Cardiac arrest.
When to See a Doctor
Immediately call emergency services if you experience:
- Chest pain lasting longer than 15 minutes.
- Discomfort that rest or medication doesn't help
- New or worsening symptoms.
Prevention of Unstable Angina
You can reduce your risk by adopting some heart-healthy habits. These are
- Regular exercise as advised by a doctor.
- Heart-healthy diet rich in fruits and vegetables.
- Avoiding tobacco and limiting alcohol consumption.
- Avoid strenuous physical exertion.
- Managing conditions like diabetes and hypertension.
- Taking prescribed medications regularly.
- If you experience unusual signs, get immediate medical help.
Conclusion
Your body sends a critical warning sign through unstable angina that needs quick action. This dangerous heart condition is different from stable angina, as it occurs without warning and points to a possible heart attack.
Quick diagnosis can save your life. A healthy lifestyle works better than treatment. Basic changes can make a big difference, like exercising regularly, eating heart-healthy foods with plenty of fruits and vegetables, and stopping smoking to lower your risk. People with diabetes or high blood pressure need to keep these conditions in check to protect their hearts.
Note that knowing the symptoms and risk factors helps you spot warning signs early and save vital minutes during a heart emergency. You can prevent most heart attack cases through awareness and active health care. Your heart never stops working for you, so it needs your care and protection through smart choices and quick medical help when needed.
FAQs
1. How is unstable angina different from stable angina?
Stable angina has a predictable pattern that occurs during activity and gets better with rest. Unstable angina strikes without warning, even during rest. The pain lasts more than 15 minutes and doesn't improve with rest or medicine.
2. Is unstable angina the same as a heart attack?
Both conditions reduce blood flow, but unstable angina doesn't permanently damage your heart. It acts as a warning sign that a heart attack could happen soon. Without treatment, about 50% of unstable angina patients have heart attacks within 30 days.
3. What are the warning signs of unstable angina?
Warning signs are:
- Chest pain that feels unusual and becomes more intense
- Chest pain happens more often
- Pain starts with little physical effort
- Breathing problems
- Sweating
- Dizziness
- Pain that spreads to your jaw or arms.
4. Who is at higher risk of unstable angina?
Your risk goes up with age (average 62 years), smoking, high blood pressure, unbalanced cholesterol, and your family's heart disease history. Black patients typically show symptoms earlier than other groups.
5. When is bypass surgery required for unstable angina?
Doctors recommend bypass surgery if you have severe blockages, especially in your left main artery or multiple affected arteries. You might need surgery if medications don't help or your heart function declines.
6. Can diabetes increase the risk of unstable angina?
Yes, diabetes by itself raises complication risk in unstable angina patients. Women with diabetes face almost twice the risk compared to those without diabetes.
7. Can unstable angina be detected on an ECG?
Yes, but not in every case. ST-segment depression or T-wave inversion on ECG might indicate unstable angina. A normal ECG doesn't rule out coronary artery disease, since only some patients show ST-segment depression at admission.





